Andrew Gallagher
Temporomandibular joint dysfunction (TMD) refers to a group of disorders affecting the joints and muscles that control jaw movement. This condition can lead to pain and difficulty moving the jaw, as well as secondary issues such as headaches and chronic facial or ear pain. It can be caused by a range of factors including:
Direct trauma: Injuries to the jaw can arise in a variety of ways, including contact sports such as football or rugby, combat sports such as boxing or martial arts, and motor vehicle accidents — whether from direct impact or whiplash.
Degenerative disease: The temporomandibular joint, like other joints in the body, can develop osteoarthritis. It can also be affected by inflammatory conditions such as rheumatoid arthritis.
Jaw alignment: Misalignment of the teeth or a poor bite can place mechanical stress on the jaw, leading to pain and dysfunction. Common dental or orthodontic treatments can sometimes have a similar effect. In my clinical experience, TMD is not uncommon following wisdom tooth extractions, particularly when the extraction has been difficult.
Muscle strain: Overuse of the jaw muscles — caused by excessive chewing, or biting down hard on something like a nut or ice cube — can trigger an acute muscle strain. Activities involving sustained jaw movement at its limits, such as singing, can also lead to TMD. As a result, TMD can affect both professional and amateur performers and may complicate voice disorders that are common in this group.
Stress and anxiety: Jaw clenching or teeth grinding is a common response to psychological stress. It often develops without the person being aware of it and tends to be worse at night.
Dental pain: This can arise in two ways — sensitivity caused by teeth grinding, or pain referred to the teeth from tight, overworked jaw muscles.
Chronic poor posture: A pronounced head-forward posture, often associated with prolonged sitting, affects how the jaw joint surfaces meet and leads to increased muscle tension in the jaw.
Symptoms of TMD
TMD presents with a wide range of symptoms, including:
- Jaw pain, often accompanied by clicking or popping sounds when opening or closing the mouth.
- Limited jaw movement, particularly when opening wide. This can affect chewing and may lead to difficulty swallowing.
- Facial pain, particularly around the jaw and temples. Pain referred from tight jaw muscles can also spread into the forehead and cheek areas, sometimes mimicking the pain of sinus problems.
- Headaches — the forehead and temple pain described above, combined with the neck tension that often accompanies TMD, is frequently experienced as a typical tension headache.
- Ear pain — because the jaw joint sits very close to the ear canal, pain from the joint is often felt as earache. If the joint is particularly tight or swollen, it may feel like a blocked or full ear.
Treatment Options
Because TMD is both complex and varied in its causes, treatment may involve several different approaches and more than one specialist. Getting the right diagnosis is the essential first step. As outlined above, TMD can mimic a range of other conditions — including sinusitis and migraine — which often leads to early misdiagnosis. Ear pain from TMD in particular can closely resemble an ear infection; in these cases, antibiotics are ineffective and patients are often referred to an ear, nose and throat specialist before TMD is identified. Once a definitive diagnosis is made, treatment options can include:
Dental care: This may include a mouth guard to protect the teeth from grinding. In some cases, orthodontic work may be needed to properly align the teeth and jaw.
Physiotherapy: This is probably the most commonly used treatment for TMD. Because the jaw muscles are the main source of pain, techniques that address muscle tightness are particularly effective — including dry needling, stretching, and therapeutic massage. A tailored exercise programme to improve both joint and muscle movement is essential for lasting relief and improved jaw function. Postural advice is often included to address any associated neck and shoulder pain.
Medication: Getting on top of pain early is important. In most cases, over-the-counter medicines such as ibuprofen or paracetamol are sufficient. A short course of muscle relaxants may occasionally be needed for persistent spasm, and a corticosteroid injection into the joint may be considered where there is significant inflammation.
Self-care: Helpful strategies include applying moist heat, avoiding hard foods by switching to a softer diet, and keeping up a regular exercise routine.
Conclusion
Temporomandibular joint dysfunction can significantly affect quality of life, but with the right diagnosis and a comprehensive treatment plan, symptoms can be managed effectively. If you suspect you may have TMD, it’s important to consult a healthcare provider for a proper assessment and personalised treatment.Andrew Gallagher is a Physiotherapist at Springs Medical , Senior Therapist The Ballarat Craniomandibular Rehabilitation Clinic (A Specialised clinic for the treatment of TMD and associated Oro Facial Pain)
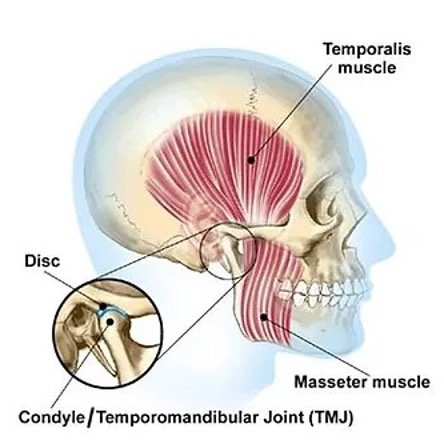
Image sourced from: https://www.radiantphysiotherapy.ca/tempomandibular-joint-dysfunction